As we know all too well by now, a novel epidemic began in the city of Wuhan in Hubei, China, in late 2019. The previously unknown organism responsible – a highly contagious coronavirus – was named COVID-19 by the World Health Organization (WHO) in February 2020 [1,2]. Previous coronavirus epidemics have included the deadly severe acute respiratory syndrome (SARS) [3,4] and the Middle East respiratory syndrome (MERS) [5,6,7].
More than a year later, the COVID-19 pandemic has decimated economies and overloaded healthcare systems around the world. As of early December 2020, nearly 70 million COVID-19 cases had been reported across 188 countries and territories, resulting in an estimated 1.6 million deaths [8].
COVID-19 patients exhibit a wide range of symptoms, including cough and difficulty breathing [9]. They may also exhibit other symptoms, such as:
- fever
- chills
- repeated shaking with chills
- muscle or body aches
- headache
- sore throat
- new loss of smell and taste
- congestion or runny nose
- nausea or vomiting
- diarrhea
Most infected people are either asymptomatic or have mild symptoms. However, a small but significant proportion of COVID-19 patients become critically ill [10] and died. Many of these latter patients did not exhibit severe symptoms initially, but then went on to develop acute respiratory distress syndrome (ARDS) and multiple-organ failure while in the later stages of the disease, or sometimes even while recovering [11].
In acute respiratory distress syndrome (ARDS), there is widespread inflammation in the lungs. Fluid collects in the air sacs or alveoli, leading to oxygen deprivation. Symptoms of ARDS include shortness of breath, rapid breathing, and bluish skin color.
Person-to-person spread of the COVID-19 virus takes place when an uninfected person comes into close contact with an infected person and is exposed to coughing, sneezing, respiratory droplets or aerosols. These aerosols may contain either virus particles or liquid respiratory droplets containing virus particles and can enter the lungs via inhalation through the nose or mouth [12].
COVID-19 and Vitamin D: Is There a Connection?
COVID-19-related deaths have been higher in some countries and populations than others. The relative proportion of elderly people, accessibility and quality of healthcare, as well as socioeconomic factors are partly responsible for these differences [13].
An important factor that appears to influence the outcome of COVID-19 infections is vitamin D status. Elderly people and others who are likely to be vitamin D deficient appear to be at greater risk for poorer outcomes.
Back in 1981, a general practitioner known as Robert Edgar Hope-Simpson had proposed that a “seasonal stimulus” closely linked to the sun’s rays might explain the seasonality of flu epidemics [14].
We now know that ultraviolet-B radiation in the sun’s rays triggers vitamin D production in the skin. Vitamin D deficiency is a common winter phenomenon, especially in northern latitudes, so perhaps it’s not a coincidence that COVID-19 started to spread in Northern Europe in the winter of 2019.
In these countries, as well as in Italy and Spain, elderly people – who are more likely to be vitamin D deficient – were seen to be the most vulnerable to COVID-19 [15]. Indeed, some aspects of COVID‐19 infections, such as excessive blood clotting, seem to get less severe in the summer [16].
People with darker skin, who are more likely to be vitamin D deficit, have had poorer outcomes when infected with COVID-19. Finally, as the exception that proves the rule, Nordic countries in Northern Europe have had exceptionally low mortality rates, possibly because many foods in these countries are fortified with vitamin D [17,18].
Vitamin D deficiency has previously been shown to increase the risk of acute respiratory disorders. Also, people infected with COVID-19 are more likely to suffer serious consequences, the older they are and if they already have chronic diseases, known as comorbidity. Both aging and comorbidity have previously been linked to lower vitamin D levels [19].
Vitamin D Deficiency and Upper Respiratory Infections: What We Know So Far
Lack of sun exposure and vitamin D deficiency has previously been linked to a greater risk of developing autoimmune diseases, cardiovascular disease, and cancer [20].

Low vitamin D status is also associated with a greater susceptibility to infectious diseases, especially upper respiratory tract infections. For instance, a 2017 meta-analysis of individual data of over 11,000 participants from 25 randomized, double-blind, placebo-controlled trials [21,22] showed that vitamin D2 or D3 supplementation protected against acute respiratory tract infections.
Interestingly, patients with very low (less than 10 ng/mL or 25 nmol/L) levels of vitamin D were seen to gain the most benefits from supplementation.
Similarly, a randomized, double-blind, placebo-controlled trial showed that schoolchildren who were given vitamin D3 supplements daily were significantly less susceptible to both flu and asthma attacks [23].
Vitamin D deficiency has been shown to contribute to acute respiratory distress syndrome (ARDS) [24]. The likelihood of a fatal outcome increases with age and with the presence of chronic diseases – both of which, as we have already seen, have been linked to lower vitamin D levels.
Vitamin D and Immunity
Vitamin D is essential for the efficient absorption of calcium and phosphate, both of which are needed for bone growth and maintaining bone strength. More recent research shows that vitamin D also plays a role in determining your risk of developing cancer and diabetes, as well as cardiac and gastrointestinal diseases [25].
Vitamin D3 or cholecalciferol is the form that is made in your skin in response to sunlight. Vitamin D3 is converted to 25-hydroxyvitamin D or calcidiol (the storage form of vitamin D) in the liver. In your kidneys – but also in alveolar cells and macrophages in the lungs – calcidiol is converted to the active form, 1, 25-dihydroxyvitamin D or calcitriol [26].
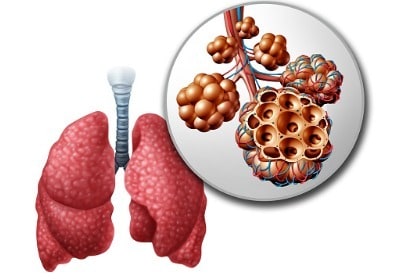
Alveoli are tiny air sacs in your lungs that take up oxygen from the air you breathe, in exchange for carbon dioxide. Alveolar cells play a role in this exchange. Macrophages are large, specialized immune cells that recognize, engulf, and destroy infected, cancerous, damaged, and dead cells.
The extent of “local” vitamin D activation in alveolar cells in the lungs has been shown to be directly related to the body’s ability to fight off acute respiratory infections [27,28]. Vitamin D triggers multiple antibacterial and antiviral actions of immune cells [29,30]. On the other hand, vitamin D deficiency reduces the immune system’s ability to fight off bacterial and viral invasions [31].
Specifically, vitamin D helps the body fight viral infections in multiple ways:
- It stimulates the production of small proteins or peptides in immune cells and in the cells lining the inner walls of our airways. These peptides have been shown to slow or even shut down viral replication, making upper respiratory viral infections – including COVID-19 – less likely to occur [32,33].
- Vitamin D lowers levels of pro-inflammatory immune signaling molecules known as cytokines, which trigger inflammation that injures the lungs in upper respiratory tract infections, leading to pneumonia. Vitamin D also increases levels of anti-inflammatory cytokines [34].
- Finally, vitamin D appears to tone down the aggressive, hyperactive immune response known as a “cytokine storm.” Although cytokine storms seen in COVID-19 patients may be different from those seen in other health conditions [35], they have nevertheless been linked to a greater likelihood of lung injury, multi-organ failure, and poorer health outcomes in critically ill COVID-19 patients [36].
Low Vitamin D Is An Independent Risk Factor for Covid-19
In a study of nearly 500 people, the relative risk of testing positive for COVID-19 was seen to be nearly twice as much for patients who were deficient in vitamin D, compared to patients who had sufficient vitamin D levels [37].
Further, based on a study involving 782 COVID-19 positive patients and 7,025 COVID-19 negative patients, Israeli scientists have concluded that a low vitamin D level is an independent risk factor for COVID-19 infection and hospitalization [38].
According to Dr. Eugene Merzon, the lead author of the study:
“The main finding of our study was the significant association of low plasma vitamin D level with the likelihood of COVID-19 infection among patients who were tested for COVID-19, even after adjustment for age, gender, socio-economic status and chronic, mental and physical disorders.”
Severely ill COVID-19 patients who required intensive care were seen to have higher levels of inflammatory markers, be much more likely to be deficient in vitamin D, and much more likely to die, than were asymptomatic patients [39].
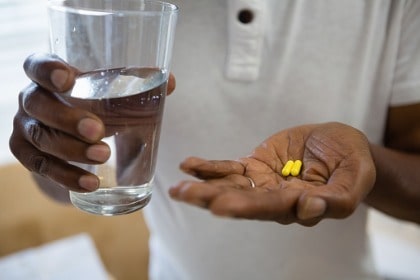
In a small-scale clinical trial, asymptomatic or mildly symptomatic patients supplemented daily with a high dose (60,000 International Units, or IU) of vitamin D3 for 7-14 days were shown to be significantly more likely to test negative for COVID-19 than patients in the control group [40].
The evidence indicates that the odds of COVID-19 patients having a mild clinical outcome increase when vitamin D levels increase – and the odds of having a critical outcome increase when vitamin D levels decrease [41]. Further, raising vitamin D levels is likely to improve clinical outcomes and prevent adverse outcomes.
Professor Rose Anne Kenny of Trinity College Dublin, the lead investigator of the Irish Longitudinal Study on Ageing (TILDA), has stated that public health bodies in the UK should recommend that everyone take vitamin D supplements during the pandemic, especially care home residents [42,43]. According to her, “The circumstantial evidence is very strong”.
Adrian Martineau, lead author of the 2017 meta-analysis describing the effects of vitamin D supplementation on the risk of developing upper respiratory tract infections has stated:
“At best vitamin D deficiency will only be one of many factors involved in determining outcome of COVID-19, but it’s a problem that could be corrected safely and cheaply; there is no downside to speak of, and good reason to think there might be a benefit” [44].
Dozens of Clinical Trials Assessing Role of Vitamin D in Covid-19 Management

More and more health experts now agree that vitamin D supplements are likely to offer a relatively easy option to decrease the impact of the COVID-19 pandemic [45]. In late Dec 2020, more than 100 scientists and doctors sent an open letter to world leaders warning of the danger of vitamin D deficiency [46].
There are also currently more than 60 clinical trials being conducted all over the world to assess the role of vitamin D in COVID-19 management [47].
One such randomized, open-label, double-masked clinical trial concluded that in patients hospitalized due to COVID-19, a high dose of vitamin D significantly reduced the need for intensive care [48].
Some researchers have even suggested that vitamin D might be a better, safer, and cheaper option than commercially available drugs used in patients with severe COVID-19 infections [49].
Vitamin D: What Is Sufficient?
Vitamin D levels between 20-50 ng/mL (30-125 nmol/L) are considered normal for the average adult. A person is considered insufficient if their vitamin D levels are between 12-20 ng/mL or 30-50 nmol/L. In adults, deficiency (less than 12 ng/mL or 30 nmol/L) can lead to osteomalacia or softening of the bones and osteoporosis (“porous bone”), a bone disease in which bones become weak and brittle.
The people most likely to have less than ideal vitamin D levels include:
- infants
- the elderly
- people with dark skin people
- city-dwellers who work mostly indoors
- people who live in countries in the northern hemisphere above 37 degrees of latitude
- the overweight and obese
- people with insulin resistance or who are diabetic
- people with chronic inflammatory conditions
- smokers
Not surprisingly, all of these people, especially the elderly, tend to have worse than average outcomes when infected with COVID-19.
To reduce the risk of COVID-19 infection, experts are now recommending that an adult take 10,000 IU per day of vitamin D3 for a few weeks to rapidly raise their levels, followed by a maintenance dose of 5,000 IU per day.
Their goal should be to raise vitamin D levels to between 40-60 ng/mL (100-150 nmol/L). For people infected with COVID-19, even higher doses might be useful.
Commercial supplements are available either as vitamin D2 or D3. Vitamin D2, also known as ergocalciferol, is typically found in mushrooms such as portobello and shiitake. Vitamin D3 is naturally present in fatty fish such as cod, swordfish, tuna, mackerel, and salmon. Milk is not a natural source, but in the U.S. milk is fortified with vitamin D, as are some yogurts, breakfast cereals, and fruit juices.
Some Considerations When Taking Vitamin D
The more vitamin D you consume, the more calcium ends up in your blood. Calcium buildup can lead to its accumulation in soft tissue such as kidneys and blood vessels – a process known as calcification, which increases the risk of chronic diseases.
Taking supplementary vitamin K2 along with vitamin D ensures that excess calcium ends up in the teeth and bones, where it belongs, and is a good idea especially with long-term supplementation. Both vitamin D and K2 are fat-soluble vitamins, absorbed best when consumed with a meal containing healthy fats.
Magnesium is essential for converting vitamin D into its active form. Fruits, vegetables, grains, and nuts are all excellent sources of magnesium. Alternatively, magnesium citrate can also be consumed as a supplement. Finally, both vitamin D and zinc play key roles in activating the body’s immune response. Taking them together is likely to complement their actions and provide greater health benefits.
Consult with your primary healthcare provider to have your vitamin D levels checked and always consult with your doctor before taking new supplements to ensure they are appropriate for you and your health status.
Tip: Turmeric 3D Contains 5,000 IU of Vitamin D
Each serving (2 capsules) of Turmeric 3D from Organixx contains 125mcg (5,000 iu) of vitamin D.
Turmeric 3D from Organixx provides you one of the most “bioavailable” forms of turmeric due to its unique fermentation process. This means your body experiences the maximum benefits of the purest, most potent turmeric available!

Look outside your front door in the spring and summer and odds are you’ll see bright yellow flowers popping up alongside that front lawn. If you’re like most people, you consider them pesky weeds that need to be annihilated as quickly and thoroughly as possible. But did you know know that those yellow flowers and the stubborn plants they bloom from are actually strong healing medicine? In fact, dandelion is one of the most powerful herbs for liver detoxification.
Read on to discover 6 important ways that dandelion supports liver health that may make you think twice about pulling them up (and cursing them out) the next time they appear on your lawn!
Dandelion Liver Detoxification
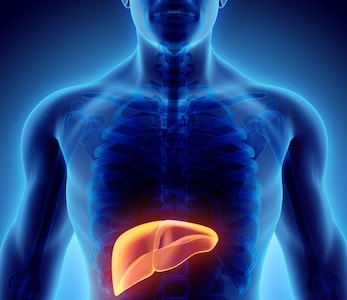
Your liver is your main organ for detoxification and your body’s primary “filter.” While it only weighs about a pound, it’s vital to your health and you’re not able to survive for long without it [1].
Without a well-functioning liver, your body isn’t able to break down fats, carbohydrates, and proteins nor is it able to get rid of pathogenic microbes and other toxins in the blood. The liver is the “metabolic center” of any living organism and is actually controlled by the central nervous system [2].
Dandelion Is One of the World’s Healthiest Foods
A 2014 study conducted by William Paterson University in New Jersey and supported by the Centers for Disease control ranked dandelion as one of the world’s healthiest foods [3]. One of the big reasons for this recognition is because of the ways that dandelion supports the liver.

Dandelion, or Taraxacum officinale, has been used for liver support and in other ways for thousands of years, especially by native cultures in North America, where it grows readily. Evidence of dandelion’s ongoing use can also be seen in China, Africa, and Western Europe [4].
So, just what is it that makes dandelion so good for the liver? The answer is as simple as the dandelion is prolific. It’s chock full of common yet essential vitamins, minerals, and phytonutrients that help to flush the liver, cleanse it, and encourage it to work at full capacity.
6 Ways Dandelion Benefits Liver Function
The liver is responsible for flushing out toxins in the body. But if it becomes overburdened, it can become a source of toxins as well. Toxic overload occurs when the liver works too hard for too long or becomes overwhelmed by too many toxins all at once.
Then the liver can become sluggish or stop working altogether, leading to a higher risk of common conditions such as kidney stones, chronic disease, or worse.
Enter the humble dandelion, which has the ability to “kickstart” the liver and help get it back in shape through several mechanisms.
#1. Dandelion’s bitter taste “kickstarts” liver function
The first way it does this is through the way it tastes. Dandelion is called a “bitter” and if you’ve ever tasted a raw dandelion leaf, then you know why.

All bitter herbs will kick in what is known as the “bitter reflex” in the body once ingested [5]. The unique phytonutrients in bitters, including certain alkaloids and sesquiterpenes, then spring into action and signal the digestive system to secrete gastric acids.
This stimulates digestive function and, in turn, all the systems connected to the gastrointestinal system, including all organs associated with the detoxification system. This includes the:
- stomach
- gallbladder
- kidneys
- pancreas
- liver
#2. Dandelion helps bile flow
Dandelion root contains high amounts of a substance called kynurenic acid. This is an amino acid that is key for bile production. In fact, a 2011 study conducted by the Institute of Agricultural Medicine in Lublin, Poland, analyzed dozens of medicinal herbs to discover the amounts of kynurenic acid in them.

Researchers found that the highest amounts were in dandelion [6]. Another study conducted by an Italian team and published in the International Journal of Immunopathology and Pharmacology found that dandelion was amongst a group of healing herbs that can be highly beneficial for the gallbladder for this same reason [7]. Kynurenic acid is also known for the support it can give to the digestive system.
#3. Dandelion helps the liver to break down and absorb minerals
Dandelion greens are a great source of key minerals, including calcium and potassium. Dandelion leaves also have high levels of vitamin A, K, and various forms of B vitamins, including folate.
Another vitamin dandelion is high in is vitamin C. Vitamin C is an important liver helper because it can assist in the breakdown of key minerals like iron. It’s also a key substance for protein synthesis and is a powerful antioxidant.
A 2003 in vivo investigation conducted by the University of São Paulo in Brazil found that vitamin C, as well as vitamin E, can help prevent and even reverse Non-Alcoholic Fatty Liver Disease [8].
#4. Dandelion is a diuretic
Flavonoids in dandelion promote increased urination, which can assist the liver in cleansing toxins out of the body at a more rapid rate [9]. This is especially beneficial when the liver needs to flush out toxins quickly, like in the case of food poisoning. Traditional cultures have used dandelion in this way for centuries.
#5. Dandelion purifies the blood
Dandelion also supports the liver by providing first-layer support for blood detoxification. It’s a great preventive for jaundice, gentle support for those who have hepatitis, and can also help with anemia since it can encourage iron absorption.
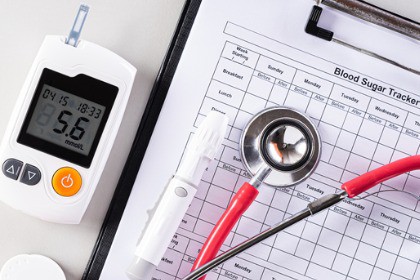
Another way that dandelion cleanses blood is by working with the pancreas to remove excess sugars. This has the added advantage of balancing blood sugar as well.
A 2005 study published in the World Journal of Gastroenterology found that dandelion may also be of benefit for those with inflammatory pancreatitis [10]. Dandelion’s blood cleansing properties can also increase balanced energy overall, according to the experts [11].
#6. Dandelion protects against drug toxicity
Finally, several studies have found that dandelion can help protect the liver from toxic overburden caused by common over-the-counter and prescription drugs. A 2012 Brazilian study was one of the first to discover the connection [12].
A 2017 Chinese investigation added more evidence. This study, which was published in the journal Molecules, found that it is the antioxidant properties of polysaccharides in dandelion that have the ability to counteract liver toxicity brought on by acetaminophen use [13].
Dandelion: A Great Liver Cleanse and More!
Remember that all the organs in your body are designed to do their job with ultimate efficiency if we can provide them with the right environment to do so. Getting dandelions in your diet in the form of tea, wild greens, or supplement form helps your liver to get back online and do its job with the greatest efficiency possible.
By now you hopefully have a greater appreciation for the common, everyday dandelion! If you have a source of clean dandelions not exposed to pesticides or road pollution, you can use all parts of the dandelion (roots, leaves, and flowers) in a wide variety of ways ranging from salads to teas.
Organixx Cleanse & Detoxx is a two-step formula that provides a gentle yet powerful full-body detox using organic botanical ingredients. Naturally purge your body of toxins, chemicals, free radicals, heavy metals, waste, as well as bacteria, and pesticides. Easily cleanse your colon, liver, kidneys, lungs, and lymphatic system resulting in increased energy, and better digestion with more nutrient absorption, in addition to improved immunity, mental clarity, and overall health and wellbeing.

Over 2 billion people around the world will drink a cup of tea today [1]. In fact, tea is the second most commonly consumed beverage after water! Whether you consider yourself a tea connoisseur or not, there’s one kind of tea you should know about if you’re at all interested in good health. It’s called matcha green tea powder and you’ll be amazed at the health benefits it has for your body – ranging from increased metabolism to improved detoxification to a stronger immune system.
What’s the Difference Between Matcha and Green Tea Powder?

All non-herbal teas – black, green, and white – come from the same plant, Camellia sinensis. What makes them different largely revolves around the timing of when the leaves are picked and how they’re processed after picking.
Matcha is green tea that is produced in its own unique way. The plants are shade-grown and the leaves are picked by hand so they are devoid of stems. Once picked, the leaves are lightly steamed and then placed in cold storage where they’re left to dry and mature. Eventually, they’re ground into a fine powder.
True Matcha Comes From Japan
Matcha green tea powder is manufactured exclusively in Japan using techniques that have been in practice for over 800 years! You may see “green tea powders” for sale that are exported from China and Korea and are typically factory processed… but they’re not true “matcha” unless produced in Japan in the traditional manner.

Because matcha green tea is created using minimal processing and little heat, the matcha green tea powder maintains a larger quantity of phytonutrients than other green teas. We’ll talk about some of these phytonutrients in the next section.
Just to give you a sneak peek at how the green tea antioxidants in matcha stack up against regular green tea…
According to a University of Colorado study, matcha green tea contains concentrations of cancer-busting epigallocatechin gallate (EGCG) that are 137 times greater than regular green tea [2]!
4 Health Benefits of Matcha Green Tea
#1. Matcha Supports the Liver with Chlorophyll
Matcha contains chlorophyll. This is the super-detoxifying substance that gives this type of tea its bright green color. Chlorophyll is known for how it can protect the liver. A substance called chlorophyllin in this phytonutrient has the ability to inhibit the mutation of key enzymes responsible for liver disease and hepatocellular carcinoma (the most common type of liver cancer in adults) [3].

Research conducted by the Linus Pauling Institute and Johns Hopkins University also found that chlorophyll can lower the risk of liver damage caused by mycotoxins (a kind of poisonous mold) in food [4]. Because matcha is produced using shade-growing techniques, the leaves are able to retain higher levels of chlorophyll than regular green tea. These amazing liver-boosting benefits are then passed on to you!
#2. Matcha Promotes Energy-Enhancing Brown Fat Cells
A 2017 Japanese trial published in the American Journal of Clinical Nutrition found that consuming matcha green tea can activate brown fat tissue. The study, which was published in the American Journal of Clinical Nutrition, discovered that when participants added matcha to their diet, the rate of energy overall that the body was able to expend rose from 10% per day to 43% per day [5].
Brown Fat Cells vs. White Fat Cells: What’s the Difference?
Believe it or not, there are good and bad kinds of fat. “White fat” is the most common kind of fat and is created when we ingest more calories than we burn. White fat cells store toxins deep inside their tissue.

When white fat accumulates around the midsection, it can be a sign of metabolic syndrome and a higher risk of chronic conditions such as:
- sleep apnea
- arthritis
- diabetes
- cancer [6]
“Brown fat,” on the other hand, is the kind you want to have around! Brown fat contains more cellular mitochondria for greater energy conversion and less “storage.” This revs up metabolism and creates heat in the body, helping you burn energy instead of just storing it [7].
According to experts, more brown fat on the body (and less white fat) is equated with greater weight loss and better efficiency of all the organs, including those having to do with detoxification [8].
#3. Matcha Green Tea Powder Is a Brain Detoxifier
When we think about detoxifying the body, we often don’t think about the toxins that are able to pass through the blood-brain barrier and make their way into our grey matter. It’s these tiny toxins, however, that are a big culprit behind the epidemic of neurodegenerative disease we see today.

According to the Alzheimer’s Association, 5 million older Americans are diagnosed with Alzheimer’s Disease each year [9]. Many more suffer from milder cognitive conditions such as brain fog and mood-related disorders like anxiety/depression.
Supporting your brain health through eating right, exercising, balancing your gut microbiome, and taking key supplements will help kickstart the process of removing pathogenic esters, gases, and the remnants of heavy metals from the nervous system and the brain area itself.
Matcha green tea can greatly help in this regard because it contains several key substances that support brain health. The hormones of stress, namely cortisol and adrenaline, act as toxins that can catalyze systemic inflammation.
This can have a direct effect on brain tissue integrity, according to researchers at the University of California, Berkeley [10]. Matcha includes a high amount of the amino acid L-Theanine, which has been proven to lower stress responses and encourage alpha brain waves [11].
Matcha green tea powder also contains a moderate amount of caffeine. Caffeine is high in antioxidants and can be a benefit for many individuals when taken in the right quantities [12].

Caffeine and L-Theanine, in the specific quantities found in matcha green tea, prove to be a winning combination for maintaining “relaxed alertness” and lowering stress-related toxins at the same time.
Finally, matcha is also neuroprotective because of certain antioxidant polyphenols that are found in all green tea, and in higher than normal amounts in matcha.
According to a 2004 study conducted by the Israeli Rappaport Family Research Institute, the polyphenols found in green tea are neuroprotective for both Alzheimer’s and Parkinson’s disease. This is due in large part because of these substances’ ability to detoxify the brain and reduce oxidative stress [13].
#4. Match Green Tea Is Super Immune-Supportive
We can’t talk about what matcha green tea powder does for your detoxification pathways without touching on its amazing benefits for the immune system as well! The immune system and the detoxification system work hand-in-hand in discovering, destroying, and eventually eliminating pathogenic (disease-causing) substances from the body.
The main component of matcha green tea responsible for fortifying immune function is the phytonutrient epigallocatechin gallate, or EGCG, mentioned earlier. EGCG has the ability to support and protect the production of T cells. It also helps the immune system fight infection directly [14].

Many researchers have analyzed the immune-supporting qualities of ECGC, especially when it comes to cancer. A 2018 study conducted by the University of Salford in England found that the amount of EGCG in matcha can actually “reprogram the metabolism of cancer cells [15].” Other research shows that ECGC can have an effect on cancer stem cells [16].
The Benefits of Matcha Green Tea Powder
If you’re a “die-hard” tea drinker and also love matcha’s unique, slightly earthy taste, then you may not have any trouble getting a cup or two of this amazing detoxifying and disease-preventing substance in your system each day.
If tea is not your thing or you’re short on time, you can still benefit from all the health advantages of matcha by using an all-in-one formula that combines matcha’s amazing properties with other key detoxifying substances such as milk thistle, dandelion, and marshmallow root.
However you decide to do it, consider adding matcha green tea to your list of “must-haves” to support detoxification and whole-body health!
Organixx Cleanse & Detoxx is a two-step formula that provides a gentle yet powerful full-body detox using organic botanical ingredients. Naturally purge your body of toxins, chemicals, free radicals, heavy metals, waste, as well as bacteria, and pesticides. Easily cleanse your colon, liver, kidneys, lungs, and lymphatic system resulting in increased energy, and better digestion with more nutrient absorption, in addition to improved immunity, mental clarity, and overall health and wellbeing.

Whether you’re a “foodie,” self-proclaimed “health nut,” or just like to be in the know about natural foods and substances that are good for the human body… the lion’s mane mushroom needs to be on your radar.
Lion’s mane is a rather unusual looking fungus with a flowing white, hair-like appearance that’s beloved as both a tasty edible mushroom and a medicinal mushroom in Japan and China. It’s also found in North America and was known to the native people who used it in powdered form for its ability to treat and heal open wounds.
Similar to many other varieties of medicinal mushrooms, lion’s mane prefers to grow on fallen hardwood trees, especially the beech tree. Its scientific name is Hericium erinaceus while it’s also commonly known as yamabushitake in Japan and hóu tóu gu in China. You might also hear it referred to by other names including:
- Satyr’s Beard
- Monkey Head Mushroom
- Bearded Tooth Mushroom
Whether you’ve never heard tell of it, or have seen it for sale at a farmer’s market or Asian food store and wondered, what is lion’s mane mushroom good for?… you’ll want to read on to discover these 7 key lion’s mane mushroom health benefits.
Lion’s Mane Mushroom Studies: What the Research Shows

Scientific research over the past few decades has demonstrated that phytochemicals (natural, plant-based compounds) found within Hericium Erinaceus have some substantial benefits for health, including significant antioxidative activity.
The key compounds that appear to be chiefly responsible for the wide range of health benefits of lion’s mane mushroom are:
- hericenones
- erinacines
- beta-glucan polysaccharides
Lion’s mane mushroom is also known to be immunomodulatory, meaning that it can stimulate or suppress the immune system to enable it to better respond to threats.
Researchers have also reported cholesterol-lowering, nerve-protecting, nerve-regenerating, anti-diabetic, and anti-cancer properties. Want to discover more about the studied health benefits of lion’s mane? Let’s dive in!
#1. Lion’s Mane and the Nervous System
While a great deal of research has been done on this unusual mushroom, the “lion’s share” of that research (if you’ll pardon the pun) has been centered around its impact on the nervous system.
The nervous system comprises the brain, spinal cord, and the nerves that travel through the body. Everything works together to send and transmit nerve impulses, which are signals that control almost every function in the human body.
When an injury occurs to the brain or spinal cord, it can take a long time to heal. Excitingly, research on lion’s mane mushroom (let’s abbreviate that to LMM) has found that it helps to speed recovery from these types of injuries.
First off, LMM stimulates the production of nerve growth factor (NGF), a protein that stimulates nerve cells to grow. LMM also has neuroprotective properties and helps regenerate damaged cells.
LMM has also been widely studied with regard to its ability to help diseases of an aging nervous system, including:
- dementia
- stroke
- Parkinson’s disease
- Alzheimer’s disease
Since pharmaceutical companies have spent billions on finding medications to cure or at least relieve the symptoms of these serious health conditions with limited success, any progress in this area is incredibly promising. It’s important to point out, however, that the research into LMM’s potential benefit for these specific diseases is still preclinical (i.e., studied in test tubes and with laboratory animals).
Many Studies into
Researchers conducting studies on lion’s mane mushroom extracts have reported the following benefits in relation to the brain and nervous system:
- Provides potent antioxidants that afford anti-inflammatory protection to nerves [1,2].
- May improve mild cognitive impairment, both in animals and in people [3-5].
- Induces the secretion of nerve growth factor (NGF), a protein involved in the regulation of growth, maintenance, and survival of nerve fibers [6-8].
- Has neuroprotective properties [9-12].
- May help protect against and ease the symptoms of Alzheimer’s disease [13-16].
- Exerts a positive influence on the fatty material that wraps protectively around nerve cells and helps to transmit electrical signals from nerve to nerve. Known as myelin, it is the loss of this protective fatty layer around nerve cells that leads to diseases like Multiple Sclerosis and other neurodegenerative diseases [17].
- May promote nerve healing and regeneration following injury [18-20].
- May ease the symptoms of diabetic neuropathy [21].
- May help protect against the progression of aging and degeneration of the nervous system [22].
- May help to prevent the death of nerve cells and brain damage after seizures or stroke [23,24].
- Is easily absorbed by the brain and body as lion’s mane compounds have the ability to cross through the protective blood-brain barrier [25].
#2. Lion’s Mane and Depression & Anxiety

Antidepressants have become one of the most widely prescribed medications across the globe [26]. The most popular variety is known as Selective Serotonin Reuptake Inhibitors (SSRIs), which enhance the neurotransmitter serotonin in the brain.
SSRIs are prescribed not only for depression but also for anxiety, eating disorders, obsessive-compulsive disorder, and a number of other mental health conditions.
A potential problem with SSRIs, however, is that they tend to come with a long list of side effects. Some of the more common SSRI side effects include [27]:
- insomnia
- skin rashes
- headaches
- muscle and joint pain
- digestive upset
- nausea
- diarrhea
- diminished sexual interest
Lion’s mane mushroom (LMM) has been reported to have anti-depressant activity, both in preclinical animal studies and human trials. The mycelia of the mushroom contain the phytochemical erinacine, which has been shown to help with the creation of neurotrophic factors in the brain [28].
Neurotrophic factors influence the growth, survival, and other functions of neurons (nerve cells). This action of erinacine has been hypothesized to play a role in depression.
Also, as noted before, LMM also stimulates the synthesis of nerve growth factor (NGF) which has an effect on brain and nervous system function [29].
A small 2010 human trial [30] found that only four weeks of taking LMM by 30 menopausal women reduced depression and anxiety in this group.
In an effort to better understand the effects of LMM on the brain and nervous system, a 2018 animal study [31] found that four weeks of administration promoted the generation of new nerve cells in the hippocampal region of the brain. (The hippocampus is involved in higher cognitive function, memory, and behavior). Researchers also found that LMM extracts reduced anxiety and depression in test animals.
Another 2018 animal study [32] reported that administration of LMM increased levels of the neurotransmitters norepinephrine, dopamine, and serotonin in the brain. LMM also blocked inflammatory pathways and regulated neurotrophic factors (as discussed above).
A 2019 human clinical trial [33] found that LMM given to 77 overweight or obese volunteers prone to binge eating decreased levels of depression, anxiety, and improved sleep after only eight weeks.
#3. Lion’s Mane and Hearing Loss
With so many studies demonstrating that LMM has profound effects on the nervous system, it’s no surprise that scientists have begun investigating if it can also help the nerves associated with hearing.

Presbycusis, the most common type of hearing loss, caused by the natural aging of the auditory system, has been shown in studies to often precede the onset of clinical dementia. Scientists also believe this hearing loss may also be an early warning signal of the onset of Alzheimer’s disease [34].
Human studies involving patients with sensorineural hearing defects (hearing loss where the root cause lies in the inner ear or the vestibulocochlear nerve) have found that the amount of circulating nerve growth factor is relatively low compared to the level found in patients with normal hearing [35].
A 2018 review of medical studies [36] investigating LMM for its effects on nerves discussed a particular study with aging mice. The results of the study indicated that the animals treated with LMM had significantly lower hearing thresholds compared with the control group. In other words, LMM helped the animals to hear better. LMM was also found to be effective in slowing hearing deterioration.
While this beneficial effect on hearing has not yet been proven in humans, it points once again to the significant beneficial role that lion’s mane mushroom is believed to have on nerve health.
#4. Lion’s Mane and the Immune System
Similar to other medicinal mushrooms like reishi, turkey tail, and maitake, lion’s mane mushrooms have important demonstrated benefits for the immune system.
Many studies [37-40] have concluded that lion’s mane mushrooms are immunomodulating agents, which means they have the ability to either stimulate or suppress the immune system (depending on what it may need) and may help the body fight infections, cancer, or other diseases.
This ability to modulate the immune system, in simpler terms, means that if the immune system is under-reacting to a threat (such as abnormal cell growth), LMM can help to augment its activity. In instances where the immune system is over-reacting, as it does with allergies and health problems like rheumatoid arthritis, LMM can act to help dampen down the immune response and inhibit its action.
#5. Lion’s Mane and the Digestive System
Many people are paying a lot more attention to their digestive health these days and for good reason. If you’re not absorbing food and nutrients properly due to digestive disorders such as “leaky gut” (intestinal permeability) or irritable bowel syndrome (IBS), you won’t be feeling as well as you might, nor operating at your best.
LMM has been shown in a number of studies to assist digestive health in several ways. Firstly, it acts as a prebiotic, providing food for and helping beneficial gut bacteria do their important work [41].
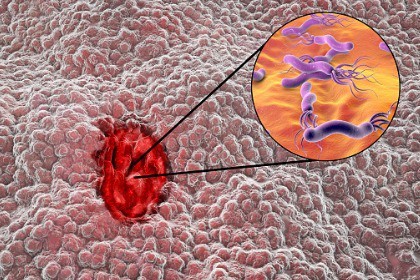
LMM also protects against the development of stomach ulcers by inhibiting the growth of a pathogen known as Helicobacter pylori which has been shown to be related to the development of stomach ulcers [42-45]. In addition, LMM exerts a protective effect on the inner layer of the digestive tract, known as the mucosa [46].
Both animal and human studies [47-53] have demonstrated that the anti-inflammatory benefits of LMM help to ease the symptoms of colitis and ulcerative colitis and other chronic inflammatory gut conditions.
#6. Lion’s Mane and Heart Health
There are a number of potential health benefits for the cardiovascular system when supplementing with lion’s mane mushroom.
Platelets are a necessary component of the blood. For instance, when you cut yourself, they keep you from bleeding to death by forming a clot at the site of the injury. However, when platelets begin to clump together abnormally, this can raise your risk of cardiovascular disease. A 2010 study [54] found that LMM inhibited the clumping of platelets.
High blood cholesterol levels can also increase the risk of cardiovascular disease. Several studies have demonstrated the ability of LMM to improve the metabolism of fats and to lower cholesterol levels [55-57].
Additionally, an in vitro (test tube) study found that LMM may help to prevent the oxidation of cholesterol in the bloodstream [58]. The importance here is that cholesterol molecules, when oxidized, can attach to arterial walls and cause them to harden. This hardening has been found to increase the risk of stroke and heart attacks.
#7. Lion’s Mane and Healthy Cell Activity
LMM may also be beneficial for promoting healthy cellular activity due to its impressive array of antioxidants, beta-glucan polysaccharides, and other phytochemicals that work in a variety of ways within the body.
Preclinical studies with cells and animals have shown that lion’s mane mushrooms have significant antitumor effects against:

- breast cancer cells [59]
- colon cancer [60,61]
- leukemia [62-64]
- gastrointestinal cancer [65-67]
- cervical cancer [68]
- liver cancer cells [69-71]
Since there have been few to no human studies performed yet utilizing lion’s mane for cancer patients, it is NOT advisable to rely solely on lion’s mane for your cancer therapy.
Combined with other treatments, however, LMM may offer some benefits for cancer patients, especially insofar as they help to modulate the action of the immune system. Animal studies to date have shown that lion’s mane mushrooms are non-toxic and safe to use [72].
Lion’s Mane Mushroom Studies Reveal Even More Potential Health Benefits
If all of the amazing Lion’s mane mushroom health benefits listed above aren’t enough, researchers have turned up even MORE potential health benefits of lion’s mane.
Here’s a quick rundown of 7 ADDITIONAL lion’s mane mushroom benefits:
- Anti-viral – A 2010 study [73] found that LMM had anti-viral properties against Human Immunodeficiency Virus 1 (HIV-1), the virus that can lead to AIDS.
- Anti-microbial – A 2012 animal study [74] demonstrated the anti-microbial properties of LMM. Researchers found that daily supplementing the feed of mice infected with Salmonella typhimurium (which can cause food poisoning – gastroenteritis, typhoid fever, or enteric fever) with LMM nearly quadrupled their life span.
- Kidney-protective – A 2013 study [75] found that LMM had kidney-protective properties.
- Liver-protective – 2015 research [76] found that LMM was liver-protective.
- Obesity-related inflammation – A 2015 study [77] found that LMM prevented or eased the inflammation released by fat tissue associated with obesity.
- Anti-diabetic – Several preclinical studies [78,79] have demonstrated the anti-diabetic, blood-sugar-lowering properties of LMM.
- Muscle endurance – A 2019 animal study [80] found that supplementation with LMM enhanced and increased muscle endurance.
Where to Get Lion’s Mane Mushroom?
If you’ve never eaten lion’s mane mushroom, there is certainly strong evidence to add this functional food into your recipe repertoire (we have some tips on cooking mushrooms here).
Fresh lion’s mane mushrooms are a bit of a specialty item that you probably won’t find on many supermarket shelves. Depending on where you live you may be able to find them in gourmet food shops, farmer’s markets seasonally, or in Asian food stores.
Because sourcing fresh lion’s mane mushrooms can be challenging (not to mention you need to be 100% assured with mushrooms that you’re getting the correct edible variety), supplementation can be a convenient alternative.
If you go this route, it’s important to work with a qualified healthcare practitioner and only purchase USDA certified organic products from a manufacturer you can trust.
Lion’s mane mushroom is one of 7 potent nutritional mushrooms found in Organixx 7 Mushrooms formula. The organic mushroom varieties selected for 7 Mushrooms are among the most clinically researched mushrooms on Earth, known for their immune system support and anti-aging properties.
7 Mushrooms from Organixx contains 7 of nature’s most powerful mushrooms for anti-aging, longevity, and immune support. Using centuries-old knowledge of the power of nutritional mushrooms and our breakthrough new formulation process we’ve unleashed the power of mushrooms in a way never before done.

Did our ancient ancestors know that bone broth was good for the digestive tract? They must have on some level since long before science was even “a thing,” they were cooking bones and gristle over an open fire to extract the nutritious elixirs inside.
These days researchers are discovering the direct reasons why bone broth for gut health is so valuable, including benefits for the immune system and just about everything else in the body.
If you’ve ever wondered “does bone broth really heal the gut?”… read on for 6 important ways that bone broth is good news for your gut AND your whole body!
Reason #1: Collagen
Let’s start with the most obvious reason why you’re hearing a lot more about bone broth for gut health these days… bone broth is a huge source of at least 3 types of collagen.
Collagen type 1 is the most abundant kind of collagen found in the bones and bodies of mammals, and thus in bone broth.
Not only is type 1 collagen essential for creating nails, hair, skin, and bones, it’s also found in high amounts in the digestive tract – and for good reason. This type of collagen is what the lining of our intestines, in large part, is made of.
The body uses type 1 collagen, in particular, for maintaining, repairing, and healing the intestinal lining. As far back as the early 1980s, researchers were discovering the power of collagen type 1 for repairing mucosal linings as well as rebalancing gastric juices in the stomach [1].
In 2012, a Brazilian team found that a combination of whey protein and collagen supplementation protected the GI tract against ulcerative lesions [2].
Type 2 collagen helps to build protein molecules in cartilage. It’s also highly beneficial, which is why you want to include joint bones in your broth if you make healing bone broth at home.
Finally, type 3 collagen can be thought of as a “helper substance” for collagen type 1. It’s found in large quantities everywhere type 1 can be found, including in the intestines.
Reason #2: Essential Amino Acids
In 2017, a study sponsored in part by the University of New Mexico’s School of Medicine in Albuquerque showed that people with certain digestive conditions, such as irritable bowel syndrome (IBS), maintain lower levels of amino acid levels in general [3]. The researchers also postulated that increasing amino acid content through food and supplementation could help digestive symptoms.
Bone broth contains many key amino acids that add another layer of healing for your gut. Both glycine and proline are amino acids found in bone broth that are essentials for brain and gut health [4].
Proline has been found to benefit lymph tissue in the gut as well as support intestinal healing [5].
Glycine is intricately involved in digestive health as well. It helps to maintain the correct acidity levels in the digestive tract and assists in the breakdown of fatty acids from food [6].
Reason #3: Glutamine
One of the superstar amino acids for gut health is glutamine (also called L-glutamine). Another reason why bone broth is so amazing for healing digestion is that it contains high concentrations of this substance.

The body requires approximately 20 essential amino acids to create the proteins which allow your body to function in a healthy way. L-Glutamine is one of these essential amino acids and is typically the most abundant amino acid in your system.
Approximately 60% of the skeletal muscle of the body is made up of glutamine and it’s important for brain and muscle health as well. The body can make it endogenously (originating internally) and it’s also found in food. Sadly, however, most people in the modern world are deficient in glutamine.
A 2017 study conducted at Rouen University Hospital in Rouen, France, found that:
“Glutamine supplementation can improve gut barrier function in several experimental conditions of injury and in some clinical situations [7].”
The researchers also noted that glutamine and other substances found in bone broth are beneficial for overall digestion.
Reason #4: Anti-Inflammatory Properties
Many compounds found in bone broth are anti-inflammatory, which can be of big benefit if you’re suffering from conditions such as diverticulitis, IBS, or Crohn’s disease [8].
Gelatin is one substance in bone broth that has been found to help calm inflammation. Gelatin is a simple substance but its power for healing lies in its ability to retain water. Ingesting gelatin in bone broth can provide another protective layer to your intestinal lining that can seal the gut and keep pathogenic (disease-causing) microbes at bay.
A 2012 Italian study discovered that both gelatin and glycine found in bone broth can reduce the inflammation that pro-inflammatory lipopolysaccharides (LPSs) are known to cause [9]. LPSs are located on the outer parts of harmful gram-negative bacteria.
(Gram-negative bacteria are often responsible for infections in healthcare settings and include Klebsiella, Acinetobacter, Pseudomonas aeruginosa, and E. coli, among many others.)

Another interesting study conducted by the Nebraska Medical Center took their cue from long-held traditional beliefs in chicken soup’s ability to “cure the common cold” and other respiratory infections.
These researchers found that both the chicken stock and the vegetable components of the soup contained substances that would cause this effect, but that the chicken stock’s anti-inflammatory components were of particular importance. In in vitro investigations, researchers found that substances in the stock, in particular, had the ability to inhibit the growth of neutrophils – pro-inflammatory immune system cells.
Reason # 5: Bone Broth for Leaky Gut & Improved Immunity
If you suffer from “leaky gut” (intestinal permeability), those mechanisms that are supposed to be protecting your digestive system from the rest of your body begin to break down.
“Tight junctions” as well as intestinal components called Glycosaminoglycans (or GAGS), which help form the tissue fibers of the intestinal lining, become defective. This allows pathogens to breach intestinal barriers, cause inflammation, and wreak havoc on your system.
Remember that up to 80% of all your immune system cells rest in the upper intestinal area of the digestive system. The connection between gut health and immune health has been confirmed by many studies over the last few decades. Likewise, the link between leaky gut and autoimmune disease has been firmly established [10].
Bone broth contains high levels of GAGs and helps to “heal and seal” the intestinal lining and heal leaky gut. When you heal the intestines, you naturally strengthen the immune system as well.
Reason #6: Vitamins & Minerals
Finally, bone broth contains dozens of other substances, including essential vitamins and minerals that are beneficial for not only the gut but for the vibrant functioning of the entire body [11].

Just some of the vitamins and minerals found in bone broth include:
- Vitamin K, which assists in the healthy flourishing of beneficial bacteria in the gut and is also needed to synthesize calcium [12]
- B vitamins, all of which help to stabilize the gut microbiome in different ways [13]
- Magnesium, essential for maintaining gut bacteria balance [14]
- Iron, also helpful for maintaining beneficial gut bacteria [15]
- Vitamin C, needed for collagen synthesis
- Vitamin A, which helps the immune system from becoming overactive [16]
Is Bone Broth Good for Your Gut? Yes!
Close to 70 million Americans are diagnosed with digestive conditions each year [17] – almost a quarter of the population! The good news is that there’s a way to help heal digestive issues before they begin to affect your whole body, through the simple act of consuming bone broth regularly.
Bone broth is truly a “superfood” that can help heal your gut and put you on the right track for optimum health. Note: if you have diagnosed gut health issues, be sure to consult with your holistic health professional for advice on how much bone broth to drink for leaky gut, acid reflux, SIBO, or IBS.
Organixx Clean Sourced Collagens blend contains five types of collagen from four sources. What’s more, it’s combined with targeted nutrients such as zinc, vitamin C, and vitamin B6 which specifically enhance the bioavailability and potency of collagen. Clean Sourced Collagens is formulated from the ground up to enhance and support your body’s natural ability to heal and rebuild itself from the INSIDE out.

For more than 2,000 years, turmeric’s rhizome (an underground stem that sends out roots and shoots) has been crushed into powder and used in Asian cookery, cosmetics, and fabric dyeing [1]. Turmeric also has a long history of use in the traditional medicinal systems of both China and India, where it is used for treating a variety of health problems. But is turmeric good for your heart? Read on to discover what science shows about turmeric and heart health.
5 Ways Turmeric Is Commonly Used as Medicine in India
As mentioned above, the cooking spice turmeric has long been revered in both traditional Indian and Chinese medicine for helping to heal a wide range of health issues.

For example, to this day in India, powdered turmeric is often consumed with boiled milk to treat cough and other respiratory ailments, as well as many digestive disorders. Meanwhile, turmeric paste is used to:
- treat eye infections
- dress wounds
- treat skin conditions including insect bites, burns, acne, and other skin diseases
1000+ Studies into the Benefits of Curcumin (Including Heart Health)
Turmeric’s longstanding popularity in traditional medicine has more recently garnered immense scientific interest.
Over the past decade or so, more than a thousand scientific and clinical studies have shown that the yellow pigment polyphenol curcumin – the predominant bioactive compound in turmeric – has powerful antioxidant, anti-inflammatory, and blood lipid management properties.
According to just one study, published in the journal Molecules in 2015,
“…chronic inflammation, oxidative stress, and most chronic diseases are closely linked, and the antioxidant properties of curcumin can play a key role in the prevention and treatment of chronic inflammation diseases” [2].
Since in this article we’re concentrating on heart health, it’s important to note that the scientific and clinical research indicates that curcumin protects the cardiovascular system in multiple ways because of its potent bioactive properties [3].
How Safe Is Curcumin?

Curcumin (which is responsible for the yellow color in turmeric) is remarkably non-toxic and shows great potential as a therapeutic agent. In fact, curcumin and other related curcuminoids have been approved by the U.S. Food and Drug Administration (FDA) as “Generally Recognized As Safe” (GRAS) [4].
Curcumin has also shown good tolerability and safety profiles in clinical trials, even at doses between 4000-8000 mg/day [5] and of doses up to 12,000 mg/day of 95% concentration of the related curcuminoid compounds curcumin, bisdemethoxycurcumin, and demethoxycurcumin [6].
Turmeric and Cholesterol: What Effect Does Curcumin Have on Blood Lipids?
Cardiovascular diseases (CVD) are complex disorders that affect blood vessels in the heart and brain. The risk for developing CVD increases with:
- overweight and obesity
- high blood pressure (BP)
- elevated blood sugar and blood lipid levels
Atherosclerosis is one of the most common causes of strokes and heart attacks. Oxidation of low-density lipoprotein (LDL) cholesterol is believed to play a critical role in the formation of so-called “atherosclerotic lesions” on the inner wall of arteries [7-9].
Promisingly, in laboratory animal studies, turmeric extract has been shown to lower levels of low-density lipoprotein (LDL) and also prevent its oxidation. Turmeric was also seen to lower total cholesterol levels while elevating levels of high-density lipoprotein (HDL) – both of which are known to further contribute to lowering heart disease risk.
How Does Turmeric Affect Lipid Levels in Humans?
In 2019, a meta-analysis and systematic review was carried out on multiple randomized controlled trials examining the actions of turmeric and curcuminoids on blood triglycerides, total cholesterol, LDL-cholesterol, and HDL-cholesterol in adults with metabolic diseases [10].
Note: A meta-analysis is a statistical analysis that combines the results of multiple scientific studies addressing the same question, with each individual study expected to have some degree of error and variation.
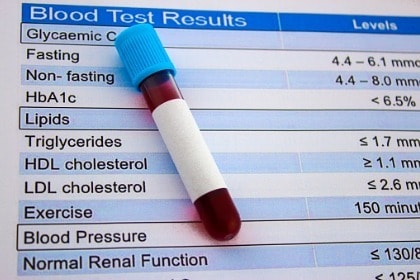
The results of this meta-analysis show that turmeric and curcuminoids significantly LOWERED total cholesterol, triglycerides, and LDL-cholesterol levels, while simultaneously elevating HDL-cholesterol levels. (HDL is what’s often referred to as the “good” cholesterol.)
In other words, turmeric and curcuminoids appear to lower the risk of heart disease in adults with metabolic diseases.
Turmeric’s Effect on Fasting Blood Glucose Levels in Patients With Metabolic Syndrome
Another meta-analysis and systematic review of seven (7) clinical trials, also published in 2019, showed similar results – turmeric improves lipid profiles, along with lowering fasting blood glucose levels in patients with metabolic syndrome [11].
According to the American Heart, Lung and Blood Institute (NHLBI) metabolic syndrome is defined as a “group of risk factors that raises the risk for heart disease and other health problems, such as diabetes and stroke [12].” These risk factors include:
- high blood pressure (BP)
- high blood sugar
- excess fat around the waist
- abnormal blood lipid levels
Interestingly, curcumin has been shown to help manage many of the risk factors for metabolic syndrome [13].

Turmeric and curcumin’s effects on blood lipids were similar to those seen in individual studies. For instance, in a randomized, double-blind controlled trial, 12 weeks of curcumin supplementation was seen to increase HDL-cholesterol levels, while significantly lowering LDL-cholesterol and triglyceride levels in patients with metabolic syndrome [14].
Similarly, in another randomized, controlled trial, bioavailability-enhanced curcuminoids were given to patients diagnosed with metabolic syndrome for 8 weeks [15].
In these patients, curcuminoids were found to be more effective than placebo in reducing levels of total cholesterol, LDL-cholesterol, non-HDL-cholesterol, triglycerides, while once again elevating HDL-cholesterol.
In yet another randomized, double-blind controlled trial, the effects of curcumin administration were assessed in 75 patients with acute coronary syndrome (ACS) [16].
ACS is a term used to describe a range of conditions associated with sudden, reduced blood flow to the heart, such as a heart attack. In these patients, turmeric was again seen to lower LDL-cholesterol and elevate HDL-cholesterol levels.
Turmeric has also been shown to lower total cholesterol and LDL-cholesterol in clinical trials with healthy subjects while raising HDL-cholesterol levels [17,18].
Turmeric’s Anti-Inflammatory Activity
Inflammation is the body’s natural response to infections and injuries – a protective immune response that removes damaged and dying cells and paves the way to begin the process of repair and healing.
Although beneficial for our body in the short term, uncontrolled high levels of inflammation are now believed to play a major role in almost every chronic disease including:
- diabetes
- heart disease
- Alzheimer’s disease
- cancer
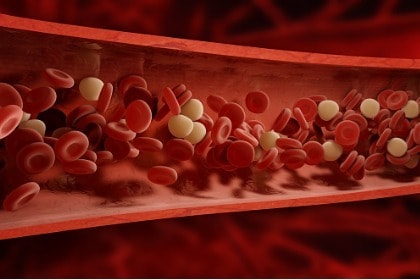
Inflammatory mechanisms have been shown to trigger aggregation or clumping together of platelets (tiny blood cells that help to form clots and stop bleeding) and blood clot formation, which prevent normal blood flow and can contribute to heart attacks and strokes. Promisingly, curcumin has been shown to interfere with platelet aggregation [19].
Chronic high inflammation has also been linked to the development of atherosclerosis, an early step in the formation of heart disease [20]. Here too, curcumin appears to be a promising candidate for the treatment of:
- thromboembolism (obstruction of a blood vessel by a clot dislodged from another site in the bloodstream), and
- atherothrombosis (disruption of the atherosclerotic lesion) [21].
Atherosclerosis associated with high levels of inflammation is commonly seen in diabetes patients. A randomized, double-blinded, and placebo-controlled clinical trial in which curcumin was given for 6 months to patients with type 2 diabetes was seen to lead to a lower risk of developing atherosclerosis and improved metabolic profiles [22].
Turmeric’s Use in Ayurveda for Inflammation & Blood Sugar Levels
As mentioned early on in this article, curcumin has a long history of use in the centuries-old traditional Indian Ayurvedic medicine. According to this ancient healing system, turmeric helps to keep inflammation at safe levels, while also keeping blood sugar within safe levels [23].

This dovetails with modern scientific research which shows that curcumin fights inflammation by interacting with multiple biological processes that play important roles in the inflammatory process [24-28].
In a 2019 randomized, placebo-controlled clinical trial reported in the journal Phytotherapy Research, curcumin supplementation was seen to significantly lower markers of inflammation in overweight and obese adolescent girls [29].
Early results from this and other clinical trials indicate that curcumin is very safe, with no toxicity observed even at very high doses [30].
Turmeric’s Impressive Antioxidant Properties
Free radicals are highly reactive chemical entities that are formed daily in our bodies because of normal, ongoing metabolic activity.
Unfortunately, when an excess of free radicals builds up, they can damage cellular structures and contribute to the development of deadly diseases such as heart disease, Alzheimer’s disease, and cancer.
Turmeric’s natural antioxidants, the curcuminoids, have been shown to neutralize harmful free radicals such as reactive oxygen and nitrogen species, minimizing the damage they cause [31,32].
Specifically, curcumin has been shown to improve markers of oxidative stress. Oxidative stress is the result of an imbalance between free radicals known as reactive oxygen species (ROS) and the antioxidant systems necessary to neutralize or detoxify them [33].

Like vitamin E, the fat-soluble curcumin is also an efficient scavenger of a type of free radicals known as hydroperoxyl [34]. Turmeric has also been shown to enhance the activities of natural antioxidant enzyme systems in the body, such as glutathione, superoxide dismutase (SOD), and others [35-37].
Thanks to its natural antioxidant capabilities and ability to detoxify harmful free radicals, turmeric and especially its curcuminoid compounds, likely reduce the risk of developing heart disease, Alzheimer’s disease, and perhaps even some forms of cancer.
5 Other Ways Turmeric is Good for Your Heart
#1. Chronic Heart Failure (CHF)
In laboratory animal studies, curcumin was seen to improve multiple molecular biomarkers of CHF [38].
#2. Diabetic Cardiomyopathy
Myopathy is a disease in which muscle fibers don’t function properly, leading to muscular weakness. In laboratory animal studies, curcumin was seen to protect against heart muscle weakness caused by diabetic cardiomyopathy [39].
#3. Cardiac Fibrosis (CF)
CF is a condition in which heart muscles become scarred and stiff because of tissue damage, disrupting electrical conduction, and eventually leading to heart failure. Cumulative evidence indicates that curcumin improves heart function in people with cardiac fibrosis [40].
#4. Cardiac Tissue Engineering (CTE)
Tissue-engineered constructs containing curcumin have been developed for managing soft tissue injuries. Similarly, some experts believe curcumin may soon be used in CTE [41].
#5. Endothelial Function
The endothelium is a single layer of cells lining the inner surface of blood vessels and lymphatic vessels in the body. Impaired endothelial function is believed to play a key role in the development of atherosclerosis, arterial hypertension, heart failure, Alzheimer’s disease, and cancer cell growth. Promisingly, curcumin appears to improve endothelial function [42].
Is Turmeric Good for Your Heart?
Getting back to our original question… “Is Turmeric Good for Your Heart?” Scientific research certainly makes a strong argument for “YES!”
But know that every substance has the potential for both positive and negative effects and that everybody (and every body) reacts differently. Be sure to check with your doctor before taking new supplements – especially if you have any pre-existing health conditions. If given the go-ahead, we recommend Turmeric 3D™ from Organixx.
With its unique fermenting processes, Turmeric 3D is the most advanced, bioavailable, and by far the most beneficial turmeric supplement available anywhere.
In addition to turmeric, it contains vitamin D3 and ginger, both potent anti-inflammatories, along with KSM-66 Ashwagandha® for reduced joint pain and to help the body recover from stress.
Turmeric 3D from Organixx provides you one of the most “bioavailable” forms of turmeric due to its unique fermentation process. This means your body experiences the maximum benefits of the purest, most potent turmeric available!







