Has Taking Antibiotics in Childhood Compromised Your Health?
In a hurry? Click here to read the Article Summary...
Many people think nothing of taking antibiotics. Yet the overprescribing of antibiotics has created a marked increase in the rise of bacterial strains that are resistant − bacteria that will not be killed by antibiotics − a problem even the U.S. Centers for Disease Control and Prevention recognizes is fast becoming a worrying public issue.
The reality is, most coughs, colds, and illnesses that affect the upper respiratory system are actually viruses, for which antibiotics are no help at all.
You see, viruses are not bacteria, thus antibiotics do not work on them. Yet, doctors continue to regularly hand out prescriptions for antibiotics, for these same sorts of illnesses that are more than likely viral infections.
The prevalence of antibiotic use and the subsequent resistant bacteria is compounding the increase of such infections (superbugs) as MRSA, and other strong, but antibiotic-resistant bacteria.
While this is bad news for patients who actually need antibiotics, the widespread use of antibiotics has other repercussions on our long-term health and, in far too many cases, they appear to begin as early as childhood.
Before we explore that, let’s take a brief look at the history of antibiotics…
Antibiotics Hailed as Wonder Drug of the Century
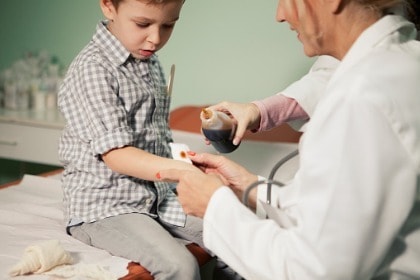
How and why has the miracle drug of WWII ended up becoming such a health hazard? It started out innocently enough. Previously, when faced with infection, people had no choice but to hope and pray, waiting to see if their bodies would win the fight with the infection, or not. A simple cut during shaving could later fester and kill you. Before antibiotics, 90% of children with bacterial meningitis died.
 Those are just two examples of how not so long ago, a simple infection could take your life, or that of someone you loved, with alarming speed. The variety of infections was countless. And other than folk medicine (old wives tales, traditions passed down through families or healers, herbs, spices, barks, etc.) there were few remedies to count on.
Those are just two examples of how not so long ago, a simple infection could take your life, or that of someone you loved, with alarming speed. The variety of infections was countless. And other than folk medicine (old wives tales, traditions passed down through families or healers, herbs, spices, barks, etc.) there were few remedies to count on.
Back then a serious infection was a bit like playing Russian roulette − would the patient survive, or not? It all depended on the body’s ability to heal, and the body’s ability to combat infection depended largely on strength of immunity − including nutrition, sanitation, and other environmental factors.
Then there were those that had to choose between death and (literally) cutting off the infected part of the body, in an attempt to stave off infection. Keep in mind, there was no anesthesia, so it was a torturous decision across the board!
Bottom line: Before antibiotics, many people, and especially children, died from simple infections. It’s understandable, then, that with the introduction of antibiotics, they were seen as a “wonder drug.” They did indeed save lives.
It was Alexander Fleming who is most widely accepted as the first to have discovered antibiotics (literally meaning “against life”), in the form of penicillin, in 1928. You have probably heard the story of the petri dishes left in the sink while the scientist was on vacation, and upon returning his discovery that molds growing on the samples had killed the bacteria he was cultivating.
Still, it took until 1945 for antibiotics to really see the light of day — Fleming’s research largely obscured by lack of interest, communication limitations, and the technology of the times. It was largely thanks to two Oxford scientists who accidentally stumbled on Fleming’s work, and the powerhouse of the war machine pushing for a viable product, that at the tail end of World War II penicillin was finally able to be produced in large enough amounts that it help save the lives of thousands that may otherwise have perished.
Fleming eventually won the Nobel prize for his work. Yet, in his acceptance speech, Fleming warned of the coming bacterial resistance we now face. But the problem even Fleming didn’t foresee (and it’s fair to say most of the medical community didn’t either), was the compounding toll of effects antibiotics have on our bodies, over time.
Is Taking Antibiotics Wiping Out Your “Good” Gut Bacteria?
It can’t be denied: antibiotics assist your body in overcoming infections more rapidly. However, a particularly overlooked and detrimental downside of taking antibiotics is that while the bacteria causing infection is being wiped out… so is an indiscriminate amount of “good” bacteria.
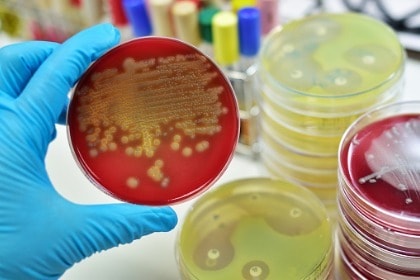 What is “good” bacteria? Those would be gut bacteria, or one type of microbiota that reside in your intestinal tract, or microbiome, as the entire ecosystem of microorganisms living inside you, is called.
What is “good” bacteria? Those would be gut bacteria, or one type of microbiota that reside in your intestinal tract, or microbiome, as the entire ecosystem of microorganisms living inside you, is called.
Within this biological system resides trillions of microbes — yeasts (and other fungi), bacteria, viruses, and more. That may sound like a bad thing, but each of these organisms, when in harmony, achieve a balance.
Having a balanced gut system allows for optimum absorption and use of nutrients (vitamins and minerals), the proper levels of serotonin and other brain chemicals, the creation of amino acids that build proteins, as well as the creation of certain vitamins and minerals. That’s just to name a few of the bodily processes that rely on good gut health.
In fact, 70% of your immune system is connected to your gut (microbiome). Scientists have also started connecting mood, cognitive function, and other seemingly unrelated body processes to the microbiome, naming it the “second brain.”
Each of the trillions of microbes are necessary — but in balance. For example, certain “harmful” bacteria act as food for yeasts that may contribute to vitamin creation, or assist in making enzymes for digestion. Or another bacteria may keep the yeasts in check, so they don’t get overgrown.
Antibiotics don’t discriminate between “good” and “bad” bacteria. They can’t choose to only target the specific infection that’s of concern. True, there are specific types of antibiotics (these days) that are better suited to attack and kill specific bacteria… but along the way, a few million other bacteria (microbiota) in your microbiome (gut) are also going to get wiped out.
That includes friendly bacteria, and others that could well be dubbed as “bad,” but exist in just enough quantities to do their job, be part of the homeostasis, and ensure your wellness.
It’s all about the synergy and balance. If one organism is given the opportunity to overpower others, disharmony ensues. This can create a chain reaction with tangible manifestations in the body, including the immune system being compromised, and other systemic disruptions that may have less than optimal results.
It’s easy to see how an imbalance in the gut can lead to a variety of health challenges.
So what does this have to do with your childhood?
Childhood Antibiotics: A Prescription for Lifelong Health Issues?
The immune system of a child, especially an infant, is a fairly delicate state of affairs. They are, naturally, immature systems. Some insist that to give infants anything but their mother’s milk is a disservice, unless they are in mortal danger.
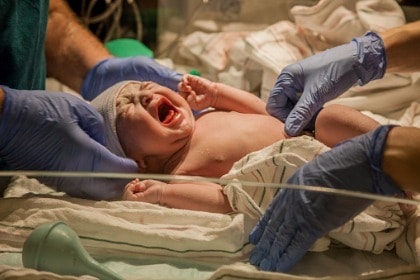 While that may be up for debate, what researchers are finding is akin to what is stated in a study published in 2015, in the journal Cell Host and Microbe. “Recent epidemiological data suggests an association between early antibiotic use and disease phenotypes in adulthood.”
While that may be up for debate, what researchers are finding is akin to what is stated in a study published in 2015, in the journal Cell Host and Microbe. “Recent epidemiological data suggests an association between early antibiotic use and disease phenotypes in adulthood.”
That is to say, that for infants and children to consume antibiotics may predispose them to future health issues. Among the connections that have been made is early antibiotic use and weaker immune systems (potentially making them susceptible to disease), as well as autoimmune issues.
Regardless, antibiotics remain the top prescription for babies. Often antibiotics are given to children for ear infections, even though the source of infection could, in fact, be a virus, not a bacteria. There is evidence that more than 80% of infections of the ear resolve themselves, without antibiotics.
At least times are changing and awareness is growing within the medical community. Even the American Academy of Pediatrics revamped their treatment guidelines for ear infections, largely due to the down sides of children taking antibiotics. Now, instead of automatically prescribing antibiotics, the AAP set the standard to be a “wait and see” protocol − for doctors to monitor infections to see if they clear up on their own.
Yet how many children reach the age of one without having had at least one prescription of these microbiota-killing meds?
It doesn’t help that these medications often come with a host of additives, artificial colorings, sugar, preservatives, and sometimes sweeteners (Splenda, among others, is known to adversely affect microbiota and the microbiome).
How Many Doses of Antibiotics Did You Take as a Child?
If you were one of those children who had repeated ear or respiratory infections as a kid, you may have been dosed with more antibiotics than you can remember. The havoc played on your microbiome would be potentially severe, depending on many outside factors that you likely didn’t have control over until adulthood.
 Even if you weren’t given a lot of antibiotics as a child, most of us have taken antibiotics at some point in our lives. Sadly, there are also antibiotics in the food chain that need to be considered, as well.
Even if you weren’t given a lot of antibiotics as a child, most of us have taken antibiotics at some point in our lives. Sadly, there are also antibiotics in the food chain that need to be considered, as well.
Antibiotics are routinely given to commercially farmed animals − poultry, cows, pigs, etc. − thus the inadvertent consumption of antibiotics through dairy products and meat.
Of course, in the case of antibiotic-filled foods, one easy solution is you can simply choose to buy and consume products that are organic, and certified antibiotic-free. However it’s a little more complicated to get your gut back into balance if it’s been compromised since childhood.
Is It Too Late to Repair My Microbiome?
The good news is that even if you have taken dozens of courses of antibiotics over your lifetime, it’s far from “too late” to rebalance your microbiome for better health. The first step, as always, is simple awareness.
If you realize now that you may have compromised your gut health through taking antibiotics, now you know. That empowers you to take action.
The top of the list of those actions would be:
#1. Stop taking antibiotics unless absolutely necessary.
Under your doctor’s supervision, make sure if you have an infection that it’s actually bacterial, before taking antibiotics. In the meantime, look for alternative ways to support a healthy immune system which will be able to fight off common illnesses.
#2. Only consume organic, antibiotic-free meat and dairy products
If you use animal products, look for those labeled as organic, pasture-raised, and antibiotic-free. The fewer antibiotics you’re purposely or inadvertently consuming, the better.
#3. Learn how to best promote a healthy microbiome.
This may include:
- Consuming fermented foods and substances
- Eating prebiotic foods (those that feed your “good” bacteria)
- A good diet with a mix of fresh organic fruits and veggies
- Taking a really good, plant-based probiotic supplement that contains a wide array of good bacteria, and other substances that support not only digestion, but your immune system
It goes without saying, but we’re saying it anyway… it can be vital to take antibiotics in the face of a truly life-threatening infection. However, everyone from the CDC to Harvard Medical School agree − only take antibiotics when truly necessary, with the full guidance of a health professional.
When you do take antibiotics, supplement with quality probiotics in order to give your “friendly,” life-giving microbiota a fighting chance to stay in balance.
And let’s not forget the basics of a healthy immune system: regular exercise, sunlight and fresh air, and an organic, well-balanced diet. Here’s to your excellent health!
Organixx ProBiotixx+ formula contains a single, super-strain of Lactobacillus plantarum, designed to help alleviate constipation… eliminate gas and belly bloat… support your entire immune system… and give you total digestive protection.

 Sources:
Sources:
Article Summary
Most coughs, colds, and illnesses that affect the upper respiratory system are actually viruses, for which antibiotics are no help. Viruses are not bacteria, thus antibiotics do not work on them.
The widespread use of antibiotics has repercussions on our long-term health and, in far too many cases, they appear to begin as early as childhood.
A detrimental downside of taking antibiotics is that while the bacteria causing infection is being wiped out, so is an indiscriminate amount of “good” bacteria.
70% of your immune system is connected to your gut (microbiome)
How you can take action to repair your microbiome:
- Stop taking antibiotics unless absolutely necessary
- Consume organic, antibiotic-free meat and dairy products
- Learn how to best promote a healthy microbiome.
Ways to promote a healthy microbiome include:
- Consuming fermented foods and substances
- Eating prebiotic foods (those that feed your “good” bacteria)
- A good diet with a mix of fresh organic fruits and veggies
- Taking a really good, plant-based probiotic supplement
When you do take antibiotics, supplement with quality probiotics in order to give your “friendly,” life-giving microbiota a fighting chance to stay in balance.




very interesting though not surprised and i mostly agree except no 2 eat antibiotic free meat and dairy surely antibiotic free food would be more accurate as this could be taken to mean we need to eat meat and dairy when in fact we dont , food being a neutral term
Thank you for sharing your input on this topic, Michael!
I have been on and off (more on) antibiotics since 1984 for a strange scalp acne. Dermatologists have diagnosed it as a form of folliculitis; impacted by inflammation. Tried numerous ointments and forms of antibiotics in an effort to try and control the acne. I’ve even been on two separate treatments of Accutane, which actually caused the acne to dissipate for 6 and 8 months respectively but eventually returned. Because of the dangers and side effects with Accutane, my current dermatologist has put me back on antibiotics (Doxycycline) at a low every other day dosage. I’ve tried to reduce the usage further by incorporating Oregano Extract Essential Oil and trying to attack the acne through a natural means for reducing inflammation. Additionally, I believe the long term use of antibiotics has greatly impacted my digestive system and bowels, and I no longer have movements unless I take Miralax and Linzess prescribed by my doctor. I was diagnosed with IBS in 1991, which I strongly believe antibiotics contributed to this condition. I also have incredible muscular back pain, which I intuitively believe is connected to my gut. If anyone has any advice with dealing with any of these issues in a more natural manner, and with results, I would be eternally grateful. Life is not very pleasant with much quality, when you have chronic scalp acne, go a week without a bowel movement and hunched over with muscular pack pain.
You may want to talk to a physician about a plant-based diet. No meat of any kind (nothing with a mother), no dairy (cheese ,, yogurt, milk products etc.) Avoid ALL oils (including Olive Oils, etc) jThere are physicians out there who embrace a plant-based life style. It may seem extreme, but there lots of recipes and cookbooks that can help you figure out what wonderful foods are available to you.
My gosh Ronald, sounds painful and difficult, have you thought of a holistic health and lifestyle coach, to support and guide you through making holistic changes? I consumed antibiotics for decades as a child with ear and sinus infections then as an adult with acne. It destroyed my micro biome and led to gall bladder disease and allergies etc. But now I am healthy all through nutrition and lifestyle changes by being coached!
I was caught up in the antibiotic nightmare. I thought antibiotics was the answer every time my allergies got bad or my glands were making me sick but actually the antibiotics were only making things worse. I hit a low with antibiotics when I just finished antibiotics then immediately went into pneumonia. Then had to fight it with essential oils. I have not had antibiotics since (14 months) which is really awesome for me. I was having antibiotics on average of three times a year. Then the Dr's telling me Kennolog shots would help with allergies. Don't do this. This is not allergy shots! You have to go see an allergist for allergy shots. Now I have been building my system up to fight off every cold and infections that go around. Herbs and essential oils heal and build your immune system. Now I'm in control.
I'm a NP and have patients try to demand an antibiotic for the
sniffles'. They will probably go to another clinic to make the demand and get it and never really understand the problems.
Too many providers are either required to make the patient happy or just don't really care about the problem because in the past they got the ABX since it took the provider only a few minutes to write and they can see more patients in a day that way. AND ' THE CUSTOMER IS ALWAYS RIGHT' philosophy is the deciding factor.
Now some are also giving Kenolog injections for the runny nose of allergies. The patients come in demanding it. When will good health be more important than big $$$$?
I also wondered about the optimax, now I am more confused as you said " Colon/Lymph 2 capsules 2 x a day in the evening and Liver/Kidney detox 2 capsules 2 times a day in the morning" so 4 in the morning nad 4 in the evening or was that a typo?
Hi Carol,
Sorry for the confusion. I edited my response to Ruth. Please review and let us know if you have further questions. Thanks!