The American Thyroid Association states that about 20 million Americans live with hypothyroidism, but the majority actually have a condition called Hashimoto’s thyroiditis [1]. This means about 14 million Americans are living with Hashimoto’s [2].
Have you or someone you loved received a Hashimoto’s thyroiditis diagnosis? Let’s explore what this condition is and important considerations along your Hashimoto’s healing journey.
What Is Hashimoto’s Thyroiditis?
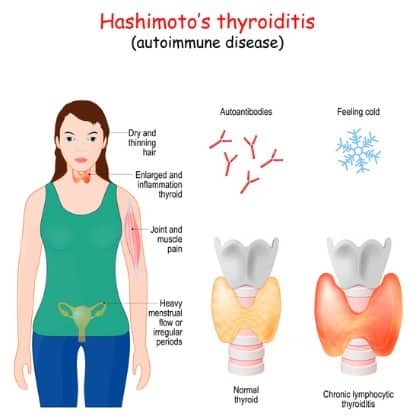
Hashimoto’s thyroiditis, also known as chronic lymphocytic thyroiditis, is an autoimmune condition with a whole laundry list of related symptoms. Although hypothyroidism is the most common, it is just one of many symptoms of Hashimoto’s [3].
Autoimmune conditions are characterized by immune system malfunctions. In most cases, antibodies are produced which “seek out” otherwise normal mechanisms in the body, destroying them and preventing them from doing their job [4].
The basic cause of Hashimoto’s is an imbalance in the function of not only the thyroid but also the pituitary and the hypothalamus caused by the autoimmune response [5].
The Impact on Gland Communication & Hormone Production
Here’s how it works: the immune system produces antibodies (thyroid peroxidase antibodies are the most common) which interrupt chemical signaling between the pituitary, the hypothalamus, and the thyroid.
Correct communication between these three glands is vital in order to ultimately produce thyroid hormones. These hormones then go on to affect hundreds of other functions throughout the body.
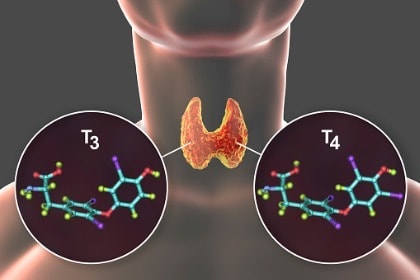
Part of the job of the pituitary gland is to produce a substance called “thyroid stimulating hormone,” or TSH. TSH’s role is to stimulate the thyroid gland into producing the thyroid hormone thyroxine (T4) as well as the metabolic hormone triiodothyronine (T3).
When Hashimoto’s mechanisms are at play, immune system antibodies intercept TSH signals before they have a chance to reach the thyroid [6].
The result is an overabundance of TSH in the bloodstream. Because the thyroid never “gets the message,” most of the time there is low thyroid production as well.
Hashimoto’s Symptoms Checklist
Some common symptoms of Hashimoto’s include:
- fatigue
- sluggishness
- dry skin
- puffiness
- constipation
- muscle weakness
- joint pain
- hair loss
- brittle nails
- excessive menstrual bleeding
- anxiety and/or depression
- heart palpitations
- cognitive decline
- loss of memory
In addition, other conditions may develop if Hashimoto’s goes on for too long untreated.
3 Conditions Related to Hashimoto’s
1. Hashimoto’s encephalopathy
Hashimoto’s encephalopathy is a neurological condition. It’s characterized by confusion, psychosis, paranoia, seizures, muscle twitches and jerks, hallucinations, and sometimes coma [7].
2. Goiter
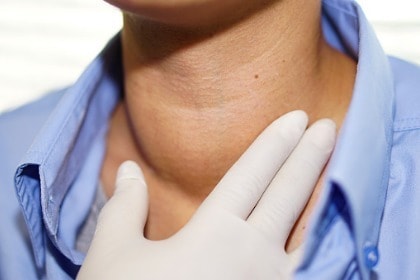
Goiter is an enlargement of the thyroid gland, either through inflammation or as a result of a nodule. It is usually visual as a lump on the front of the neck [8].
Goiter is serious because individuals with goiter may be more likely to experience a thyroid storm or “thyrotoxicosis crisis.” This is when thyroid hormone levels jump dramatically. Thyroid storm can be life-threatening if not stabilized quickly [9].
3. Hyperthyroidism
Surprisingly, at times Hashimoto’s suffers may experience the symptoms of hyperthyroidism too. Dr. Izabella Wentz is a well-known expert on Hashimoto’s who has struggled with the disease herself. [Note: Hypothyroidism is an underactive thyroid while hyperthyroidism has to do with overproduction of thyroid hormones.]
“People with Hashimoto’s may experience BOTH hypothyroid and hyperthyroid symptoms because as the thyroid cells are destroyed, stored hormones are released into the circulation causing a toxic level of thyroid hormone in the body, also known as thyrotoxicosis or Hashitoxicosis,” says Wentz.
“Eventually, the stored thyroid may become depleted and due to thyroid cell damage, the person is no longer able to produce enough hormones. At this time, hypothyroidism develops [10].”
How Do You Get a Hashimoto’s Thyroiditis Diagnosis?
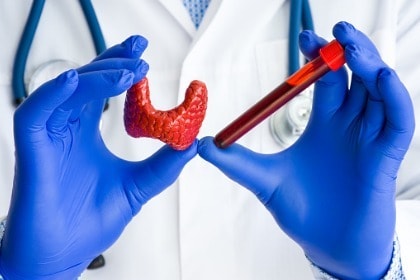
Besides relying on the wide range of symptoms, most people are presented with a Hashimoto’s thyroiditis diagnosis through a blood test which detects high TSH as well as the presence of thyroid antibodies.
Conventional Hashimoto’s Treatment
When it comes to autoimmune disease in general, many physicians simply say that they don’t know what causes it or that it’s a matter of “bad genes.” Many still feel that diet and lifestyle have nothing to do with it and that autoimmune diseases cannot be reversed.
They will often recommend prescription drugs, including low-dose chemo drugs, that focus on shutting down part the part of the immune system or reducing symptoms [11].
In the case of a Hashimoto’s thyroiditis diagnosis, the majority of Western doctors will prescribe pharmaceutical thyroid replacements such as Levothyroxine [12].
Unfortunately, thyroid medications will not fix the underlying autoimmune condition. There’s also the concern that all pharmaceuticals come with a list of at least some potential side effects.
For example, there are some scary ramifications to long-term thyroid replacement use. As far back as 1976, a study published in the Journal of the American Medical Association (JAMA) found a 200% increase in breast cancer incidence amongst women who had been on thyroid hormone replacement for at least 15 years, compared to women who were not on the drug [13].
The Link Between Breast Cancer and Thyroid Conditions
Several more recent studies have investigated the link between thyroid disorders and breast cancer. This growing body of evidence shows that breast cancer patients are more likely to also have a thyroid disorder (both autoimmune and non-autoimmune). For example, in one 1996 study, Hashimoto’s thyroiditis was observed in 13.7% breast cancer patients while only 2% of healthy controls had this autoimmune condition [14].

Research has also demonstrated that breast cancer and thyroid cancer are related. A 2016 systematic review and meta-analysis of all relevant studies stated that “There is a clear increase in the odds of developing either thyroid or breast cancer as a secondary malignancy after diagnosis with the other [15].”
The takeaway here should not be fear, but rather an awareness that a health-focused lifestyle is crucial for both a healthy thyroid and breasts.
Lowering Stress, Lifestyle Changes, and Iodine: Finding the Right Hashimoto’s Treatment Protocol
Can Hashimoto’s thyroiditis be reversed? Yes, it can! Thousands have turned Hashimoto’s around through the right kind of diet (including healing the gut and removing gluten), making lifestyle changes, lowering stress, and detoxifying the body.
When it comes to nutrients, iodine is literally the “food” for your thyroid. There are differing opinions, however, as to what role iodine should play in someone healing from Hashimoto’s.
Most in conventional medicine advise against supplementing with iodine. On the other hand, some functional medicine experts state that flooding the body with iodine is the key to healing. While some people do have success with this method, for others, taking megadoses of this essential mineral can make matters worse. This is why it’s critical that you work with a trusted healthcare provider to determine what Hashimoto’s treatment plan is best for you.

Another approach falls somewhere in the middle ground. A 1998 German clinical trial published in the European Journal of Endocrinology found that Hashimoto’s patients who took low doses of iodine (250 micrograms of potassium iodide) for four months saw “slight but significant” improvements in their thyroid hormone function [16].
Other studies point to the importance of including “helpers” for iodine absorption. Research has been conducted on the role selenium, iron, zinc, and thiamin in particular play in iodine synthesis and thyroid healing. For instance, a 2002 study conducted by the Swiss Federal Institute of Technology in Zürich stressed the importance of selenium.
“Adequate selenium nutrition supports efficient thyroid hormone synthesis and metabolism and protects the thyroid gland from damage by excessive iodide exposure,” said the researchers in the journal Thyroid [17].
All of this demonstrates, again, that there is no one clear path when it comes to treating Hashimoto’s thyroiditis. However, there is something that almost everyone can do to improve their thyroid health.
Everyone Can Benefit by Detoxing From Halide Toxins
Iodine is both an element (remember the periodic table in chemistry class?) and an essential mineral that’s critical for proper functioning of every cell in the human body. It’s especially important for the thyroid.

In women, iodine is found most in the thyroid, ovaries, breasts, and uterus. In men, it’s the thyroid followed by the reproductive system and the prostate.
Whether or not you have a diagnosed thyroid condition, your thyroid will not be able to absorb the iodine it needs if you have a high level of halide toxicity. Halides are other elements that can take up iodine receptor sites within the body, preventing iodine from getting where it needs to go.
The main halides to watch out for are:
Fluoride: found in tap water, dental cleansers, toothpastes, and mouthwashes as well as some consumer goods. A large-scale English study discovered that hypothyroidism was two times as high in areas that had fluoridated water versus areas that were not [15].
Bromide: found in swimming pools, indoor paints and plastics, as well as some foods such as commercial bread. Studies have increasingly shown that bromide may be more aggressive at blocking iodine than previously thought [16]. Bromide toxicity has been increasing significantly over recent years.

Chlorine: found in tap water, bleach, swimming pools, hot tubs, and in many kinds of plastics, dyes, and insecticides. If you never thought about the impact chlorine in pools and hot tubs can have on your health, a U.S. Environmental Protection Agency study found that kids who swam regularly in swimming pools were more prone to asthma [20].
Perchlorate: a man-made substance that has many of the same chemical components as naturally occurring halides. It is found in jet fuel and many agricultural fertilizers. A recent study by the University of California, Los Angeles, found that exposure to perchlorate may lead to a higher risk of either Hashimoto’s or Grave’s disease (aka toxic diffuse goiter) [21]. Perchlorate can be found in the bodies of just about everyone on the planet.
3 Steps to Detox From Halides
Halides are easy to eliminate from the body if you know how. The first step is to stay away from as many sources of them as you can. The second step is to get tested. Many labs offer an at-home “iodine loading” test that can also determine if you have high levels of toxic halides.
Finally, the third step is to detox. Work with a qualified healthcare practitioner if your levels are especially high. Eliminating halide sources from your environment and supplementing with a quality source of iodine (when appropriate) can slowly remove them from the body over time as well.
Nascent Iodine Is the Safest Form of Iodine for Hashimoto’s
If you have Hashimoto’s, you need to find a qualified healthcare professional who can help guide your healing. Determine with them if slowly introducing a quality iodine supplement is right for you.
Nascent iodine is the most gentle, safest form of iodine out there since it does not need to be converted in order to be absorbed in the body. It absorbs quickly and at the cellular level.
Organixx Nascent Iodine is organically sourced and does not come from kelp, so it is energy-efficient yet gentle.
If you have a Hashimoto’s thyroiditis diagnosis or other thyroid issues know that there are options for you on your healing path. Be sure to get your iodine and halide toxin levels tested and nourish yourself with essential minerals such as vital nascent iodine ONLY IF recommended by your doctor.
If you are fortunate not to have any thyroid issues currently, keep your thyroid healthy by ensuring you’re consuming enough quality foods with iodine. If you’re supplementing with iodine, make sure it’s the right kind for you.
When your organs are working hard to detoxify, you want the purest form of iodine possible to help them work more efficiently. It only makes sense to use an organic form that’s totally natural and free of chemicals. Organixx Iodine is one of the only formulas that is USDA Certified Organic. It’s a pure, nascent form of iodine which your thyroid can use immediately.




