Did you know that missing sleep on a regular basis can take years off your life? If you’re having sleep problems, not feeling refreshed when you rise in the morning, and in fact are feeling worse than when you went to bed… you might have obstructive sleep apnea. Read on to find out what causes this sleep disorder, why it should not be ignored, and what new obstructive sleep apnea treatments help.
What Is Obstructive Sleep Apnea?
Obstructive sleep apnea is a sleeping disorder where a blockage in the airways briefly interrupts breathing and/or causes natural breathing patterns to stop altogether as one sleeps.
It should not be confused with a more serious condition known as central sleep apnea which occurs when the brain fails to transmit a signal to the muscles responsible for natural breathing patterns. Central sleep apnea is most commonly seen in patients with heart failure. It requires different therapies and interventions than obstructive sleep apnea – the subject of this article.
The Long-Term Effects of Obstructive Sleep Apnea on Your Health
 Obstructive sleep apnea can be incredibly disruptive, not only in terms of altered breathing, but also causing the sufferer to feel unrefreshed after sleep, fatigued during the day, and unable to concentrate well.
Obstructive sleep apnea can be incredibly disruptive, not only in terms of altered breathing, but also causing the sufferer to feel unrefreshed after sleep, fatigued during the day, and unable to concentrate well.
And it doesn’t stop there. Studies show that obstructive sleep apnea can adversely affect multiple systems of the body. It can increase a person’s risk for heart disease, hypertension, stroke, obesity, insulin resistance, diabetes, depression, and memory problems [1].
Sleep apnea has also been associated with poor job performance, car accidents, and compromised immunity. Experts agree that obstructive sleep apnea should be treated as a chronic disease, requiring long-term, multi-disciplinary management [2].
Symptoms of Obstructive Sleep Apnea
The following are some of the most common symptoms of obstructive sleep apnea:
- Snoring
- Momentary stoppage of breathing during sleep (of which the sleeper is generally unaware, usually reported by sleep partner)
- Waking suddenly gasping, snorting, or choking
- Non-refreshing sleep
- Dry mouth upon awakening
- Frequent morning headaches
- Insomnia or difficulty staying asleep
- Hypersomnia – feeling excessively sleepy during the day
- Concentration difficulties when awake, memory loss
- Moodiness, irritability
- Decreased libido
What Commonly Occurs in Obstructive Sleep Apnea?
Air passes through the nose, mouth, and the throat on its way to the lungs. Under normal conditions, the back of the throat is soft and tends to collapse inward as a person breathes. Certain muscles then dilate (widen) to keep the airway open. If tissues at the back of the throat collapse and momentarily block airways, breathing temporarily stops, known as apnea.
If the obstruction is incomplete, the sleeper continues to breathe, but slowly and shallowly, known as hypopnea. This causes  the throat to vibrate, making the sleeper snore.
the throat to vibrate, making the sleeper snore.
Snoring often also occurs without apnea. When the sleeper stops breathing, the brain eventually registers the lack of oxygen and sends a wake-up call to breathing muscles to restart breathing.
At this point, the sleeper may start gasping or snorting but does not usually wake up completely.
In most cases, the sleeper is unaware of all this – sleeping partners tend to be the ones that report the problem. This process can occur dozens of times per night, causing unrestful, fragmented sleep. No wonder the person with obstructive sleep apnea feels fatigued and excessively sleepy during the day!
What Causes Obstructive Sleep Apnea?
There are a number of different possible causes of obstructive sleep apnea. These are some of the major ones:
- Throat Muscle Weakness – One of the most common causes, the muscles of the throat are not as strong as they should be, thus allowing a narrowing of the upper airways during sleep.
- Deviated Septum – Can cause congestion or obstruction of upper airways.
- Obesity – Studies show that obesity can be a factor in sleep apnea for both men and women [1]. Fat doesn’t just deposit around one’s middle, it also deposits around upper airways and can obstruct breathing.
- Smaller Upper Airways (“SUA”) – There are many contributory factors for SUA, but the major ones are congestion, allergies, enlarged tonsils and adenoids, and obesity
- Tongue-tie – Caused by the skin attachment known as the frenulum at the base of the tongue being too short. Tongue-ties have an impact on oral and facial development, and that in turn impacts the development of airways, making them more collapsible [3].
- Alcohol Use – Drinking alcohol can contribute to sleep apnea because it relaxes the muscles of the throat. A 2018 study found that higher levels of alcohol consumption increased the risk of sleep apnea by 25% [4].
- Smoking. Smoking has been found to create obstructive sleep apnea because it increases inflammation and fluid retention in upper airways and throat.
- Back Sleeping – Can lead to snoring and sleep apnea if some of the other contributory factors listed here are also present.
- Pregnancy – The hormones secreted during pregnancy can congest the mucous membranes of upper airways, thus increasing the likelihood of sleep apnea. High blood pressure and/or gestational diabetes can also contribute to sleep apnea during pregnancy.
- Certain Medications – Taking medications such as opioids or sedatives may cause sleep apnea because these substances also relax throat muscles.
- Mouth Breathing – According to Myofunctional Therapist Sarah Hornsby, breathing through the mouth rather than the nose sets us up for sleep apnea later in life. Mouth breathing impacts upon jaw development, allows the tongue to drop in the mouth, impacting airways and the proper structure and even growth of the jaw and maxilla, all of which can lead to sleep apnea.
- Aging – Studies show that between 13% and 32% of people over 65 years of age have some sleep apnea [5].
- Dental Conditions – A large overbite can cause sleep apnea.
- Neck Circumference – People with thicker necks often have SUA.
3 Treatments for Obstructive Sleep Apnea
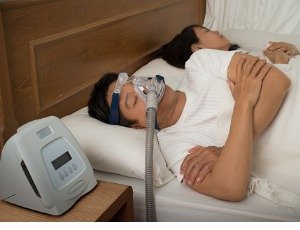 #1. CPAP
#1. CPAP
CPAP stands for “continuous positive airway pressure” and it is the gold standard of treatment for obstructive sleep apnea with a good level of effectiveness. The CPAP is a small device that delivers pressurized air at a constant and steady rate through a hose and a mask or nose piece while you sleep.
The average cost for a CPAP device is around $850 in the USA. Some insurance companies cover the cost of CPAP. For those who are uninsured, the expense of the device often makes this treatment unavailable.
#2. Mandibular Advancement Device
This is a mouth guard custom-fit to your mouth by a dentist and worn at night. The device is molded to fit both the bottom and top teeth and joins in such a way that the bottom teeth are positioned in front of the top teeth.
This pushes the lower jaw slightly forward and tightens and prevents obstruction in the soft tissues and upper airway muscles. This keeps airways open and reduces apnea/hypopnea episodes during sleep. The tightening of the airway also prevents the upper airway tissues from vibrating during sleep, which helps to minimize or prevent snoring.
A 2016 French study found that these dental devices were more efficient than CPAP for mild-to-moderate obstructive sleep apnea sufferers with low cardiovascular disease risk. However, for those who had a higher risk of cardiovascular disease, the CPAP was the better choice [6]. Again, costs can be prohibitive at around $2,000 USD for the custom-fitted device.
In the meantime, due to a growing awareness that better sleep equates to feeling better and many other associated health improvements, another more holistic and affordable treatment has been devised for people with obstructive sleep apnea.
#3. Myofunctional Therapy
This is one of the newer, better, and more affordable options for treating sleep apnea. Myofunctional Therapy involves teaching the sleep apnea sufferer breathing retraining exercises, as well as exercises to help restore normal strength and coordination of facial and tongue muscles.
According to Myofunctional Therapist Sarah Hornsby, there are four main goals of this therapy:
- Breathing through the nose. Because mouth breathing is one of the main causes of sleep apnea, it’s important to deal with
 the conditions that cause us to breathe through our mouths. These might include allergies, asthma, colds, and recurrent sinus infections.Dietary changes may need to be employed, along with the use of a neti pot to rinse out the sinuses and working with an allergist or ENT specialist. All of these can be beneficial to help clear nasal congestion.
the conditions that cause us to breathe through our mouths. These might include allergies, asthma, colds, and recurrent sinus infections.Dietary changes may need to be employed, along with the use of a neti pot to rinse out the sinuses and working with an allergist or ENT specialist. All of these can be beneficial to help clear nasal congestion. - Keeping lips together, termed a “lip seal.” This goal is only achievable after the first goal has been met. Some therapists even recommend using a particular type of sticky tape to seal the lips shut, in order to avoid mouth breathing at night and its associated problems.
- Tongue resting at the roof of the mouth. Rather than the tongue sitting at the bottom of the mouth, it should be resting and making contact with the soft palate at the top of the mouth. Exercises are given to help sleep apnea sufferers achieve this goal.
- Swallowing properly. Many of us do not swallow as we were designed to do, compromising the integrity of teeth and other structures. Learning to swallow properly can contribute to better sleep.
Hornsby explains that the ripple effect of achieving these four goals is enormously significant for anyone suffering from obstructive sleep apnea. Other lifestyle changes that can positively impact obstructive sleep apnea include:
- Avoidance of Smoking, Alcohol, and Sedatives – All three of these have been shown to interfere with the quality of sleep. They are also known to relax the throat muscles, the uvula, and palate, all of which are required to help control breathing. Alcohol and smoking also contribute to inflammation and fluid retention in airways, which further compromises airways.
- Striving for a Healthy Weight – If you are overweight or obese, work with someone who can help you lose this weight. This is a crucial step because not only can obesity lead to sleep apnea, lack of sleep can also make it harder to lose weight. Obesity also contributes to many of the same diseases that sleep apnea does.
- Dealing with Acid Reflux – When a person suffers from acid reflux, what often happens is that acid from the stomach travels up the esophagus and into the throat and voice box. This causes irritation and inflammation of muscles in the throat, increasing the likelihood of snoring and sleep apnea.By adjusting the diet to less acidic foods, and (where needed) working with a healthcare practitioner to repair a faulty or damaged esophageal sphincter, this problem can be solved.
(It’s important to note that while many people blame that burning sensation in their esophagus on too much stomach acid, low stomach acid is actually far more common and causes similar painful symptoms.)
- Adjust How You Sleep – Avoid sleeping on the back. This position presses the tongue and palate against the back of the throat and generally makes snoring and apnea worse. Sleeping on one’s side and using a pillow that slightly elevates the head often helps to alleviate sleep apnea symptoms.
Obstructive sleep apnea is a complex problem that can lead to additional health issues. Whether you choose to see a doctor, a dentist, or a myofunctional therapist, just be sure to seek assistance for this problem sooner rather than later.
Magnesium deficiency is linked to stress, diabetes, heart disease, osteoporosis, chronic fatigue syndrome, depression, anxiety, trouble sleeping, sore muscles, migraines, and many more debilitating health conditions.
If your body needs magnesium, you want the most beneficial kind your body can actually absorb. Organixx Magnesium 7 gives you seven (7) of the very best, most bioavailable types of elemental magnesium available.




